Andropause: Roy’s Story
It’s August 5th, Roy’s 52nd birthday. The cake has been baked, the presents wrapped. But Roy just doesn’t feel like celebrating. His family and friends know him as active, outgoing and ambitious. He’s VP of Purchasing for an electronics firm, he coaches his son’s hockey team and he’s the one who gets the call when there’s a charity car wash to organize. His wife Ellen has always been his best friend. Their lives revolve around teenaged kids and friends. There are dinner parties, outings, and on weekends he plays tennis or works on his 9 handicap.
But lately, Roy has not “been himself”. He always feels used up at the end of the day. The old drive is missing. After dinner, all he can think about is hitting the sofa with the remote, often dozing right there. His relationship with Ellen has also been strained. They often argue now and he tends to just clam up more. He doesn’t feel much like having sex anymore either. In fact, it’s been weeks now.
At work, he feels oddly threatened by his bright new assistant who would obviously like his job. He no longer feels so sure of himself or his future. His co-workers have noticed that he is edgy and often unreasonable in his demands. “The golf game tomorrow? How can I get out of it? I’m just too tired to go. I just don’t have the same enthusiasm for things. Ah, I don’t know, I must be getting old.”
Sound Familiar?
Roy isn’t just “getting old”. He’s going through Andropause, often referred to as “male menopause.” And there’s plenty he can do about it to feel fit and energetic again – and get his positive outlook back.
If Roy’s story sounds familiar to you, you may want to take a short quiz on page 4 to see if you might also be going through Andropause.
The existence of Andropause is now recognized by the medical world – including the Canadian Andropause Society – and by Canadians alike.
In fact, a recent Angus Reid survey found that 70% of the general public share the belief that men experience a mid-life stage similar to women’s menopause. Andropause (also called “male menopause”) is a normal part of aging; although, for some men it is accompanied by a gradual and undesired decline in their sexuality, mood and overall energy. Sometimes it can even expose men to more serious health risks.
As with women, Andropause begins at a time when life often offers some of its greatest rewards. This site has been designed to arm you with actionable information about Andropause – what causes it and what you can do about it. And if you are going through Andropause, we hope this information will help you maintain a healthy and active quality of life throughout your middle-years. For immediate answers to your questions, click on Your Questions below.
Are you, or is someone you love, showing the telltale signs of the Andropause? Before reading on, click on our rapid quiz to find out.
By the time men are between the ages of 40 and 55, they can experience a phenomenon similar to the female menopause, called Andropause. Unlike women, men do not have a clear-cut external signpost such as the cessation of menstruation to mark this transition. Both, however, are distinguished by a drop in hormone levels. Estrogen in the female, testosterone in the male. The bodily changes occur very gradually in men and may be accompanied by changes in attitudes and moods, fatigue, a loss of energy, sex drive and physical agility.
What’s more, studies show that this decline in testosterone can actually put one at risk of other health problems like heart disease and weak bones. Since all this happens at a time of life when many men begin to question their values, accomplishments and direction in life, it’s often difficult to realize that the changes occurring are related to more than just external conditions.
Unlike menopause, which generally occurs in women during their mid-forties to mid-fifties, men’s “transition” may be much more gradual and expand over many decades. Attitude, psychological stress, alcohol, injuries or surgery, medications, obesity and infections can contribute to its onset.
Although with age, a decline in testosterone levels will occur in virtually all men, there is no way of predicting who will experience Andropausal symptoms of sufficient severity to seek medical help. Neither is it predictable at what age symptoms will occur in a particular individual. Each man’s symptoms may be also different.
The role of testosterone
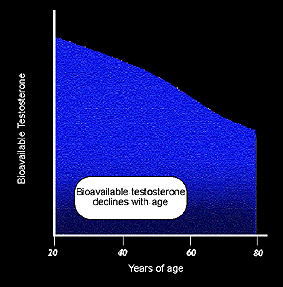
Starting at about age 30, testosterone levels drop by about 10 percent every decade. At the same time, another factor in the body called Sex Binding Hormone Globulin, or SHBG, is increasing. SHBG traps much of the testosterone that is still circulating and makes it unavailable to exert its effects in the body’s tissues. What’s left over does the beneficial work and is known as ‘bioavailable’ testosterone.
Andropause is associated with low (“bioavailable”) testosterone levels. Every man experiences a decline of bioavailable testosterone but some men’s levels dip lower than others. And when this happens these men can experience Andropausal symptoms.
These symptoms can impact their quality of life and may expose them to other, longer-term risks of low testosterone. It is estimated that 30% of men in their 50s will have testosterone levels low enough to be causing symptoms or putting them at risk.
Why is testosterone so important?
Testosterone is a hormone that has a unique effect on a man’s total body. It is produced in the testes and in the adrenal glands. It is to males what estrogen is to females. Testosterone helps to build protein and is essential for normal sexual behavior and producing erections. It also affects many metabolic activities such as production of blood cells in the bone marrow, bone formation, lipid meta-bolism, carbohydrate metabolism, liver function and prostate gland growth.
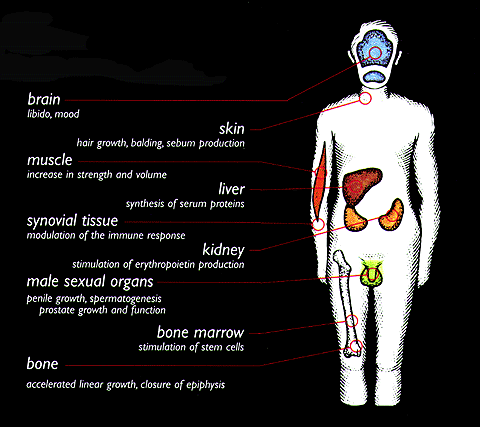
Impact of low bioavailable testosterone
When there is less testosterone available to do its work, the testosterone target organ response decreases, bringing about many changes. There is great variability in testosterone levels among healthy men so not all will experience the same changes to the same extent. But typical responses to low bio available testosterone levels include:
- Low sex drive
- Emotional, psychological and behavioral changes
- Decreased muscle mass
- Loss of muscle strength
- Increased upper and central body fat
Is Andropause a new phenomenon?
Yes and no. In fact, Andropause was first described in medical literature in the 1940’s. So it’s not really new. But, our ability to diagnose it properly is. Sensitive tests for bioavailable testosterone weren’t available until recently, so Andropause has gone through a long period where it was under-diagnosed and under-treated. Now that men are living longer, there is heightened interest in Andropause and this will help to advance our approach to this important life stage which was identified so long ago.
Diagnosing Andropause
Another reason why Andropause has been under-diagnosed over the years is that symptoms can be vague and can vary a lot among individuals. Some men find it difficult to admit that there’s even a problem. And often physicians didn’t always think of low testosterone levels as a possible culprit. So these factors often lead doctors to conclude that symptoms were related to other medical conditions (i.e. depression) or were simply related to aging and often encouraged their patients to accept that “they were no longer spring chickens”. But this situation is changing. New blood testing methods are available and there is a increased interest in men’s’ aging among medical researchers. In fact, so much attention is being focused on Andropause that major efforts are underway to quickly share emerging scientific information with Canadian physicians.
Am I going through Andropause?
Take this test and take the first step to feeling better.
- Do you have a decrease in your sex drive (libido)?
- Do you have a lack of energy?
- Do you have a decrease in strength and/or endurance?
- Have you lost height?
- Have you noticed a decreased “enjoyment in life”?
- Are you sad and/or grumpy?
- Are your erections less strong?
- Have you noticed a recent deterioration in your ability to play sports?
- Are you falling asleep after dinner?
- Has there been a recent deterioration in your work performance?
Of course, every person is different. And not all men going through this stage of life will experience it exactly the same way. The passage into middle age is a complicated phase. It’s full of changes at all levels – personal, social, economic, family, etc. It may therefore be difficult to differentiate these changes from the symptoms of other conditions that can create some of the same symptoms.
Nevertheless, if you did answer “Yes” to 1 or 7 or to any three questions in all, it would be worthwhile discussing these symptoms with your physician. He/she may then have your bioavailable testosterone level checked.
Why should Andropause be taken seriously?
Apart from the impact that Andropause may have on your quality of life, there are other longer-term and silent effects of Andropause that are harder to track: increased cardiovascular risk and osteoporosis.
Andropause & Osteoporosis
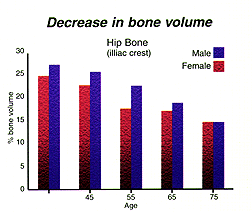
In a healthy individual, bone tissue is constantly being broken down and rebuilt. In an individual with osteoporosis, more bone tissue is lost than is regenerated. We’ve all heard of women suffering from weaker bones, or osteoporosis, after menopause. In men, testosterone is thought to play a role in helping to maintain this balance. Between the ages of 40 and 70 years, male bone density falls by up to 15 percent.
Unfortunately, with advancing age and declining testosterone levels, men seem to demonstrate a similar pattern of risk for osteoporosis as women. What’s more, approximately one in eight men over age 50 actually has osteoporosis. The incidence of hip fractures rises exponentially in aging men, as it does in women, starting about 5 to 10 years later than in women. In Canada, 20-30% of osteoporotic fractures occur in men. The incidence in fractures has been increasing in men, whereas it seems to be stabilizing in women Ñ likely due to the lifestyle changes, calcium supplements and hormone replacement therapies that women are embracing.
Why should I worry about osteoporosis?
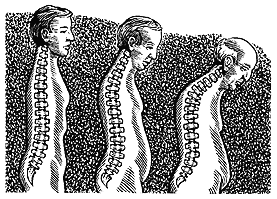
Low bone density puts one at risk of frequent fractures, associated pain, and in many cases, loss of independence. Wrists, hips, spine and ribs are most commonly affected. The consequences of osteoporosis are often seen as a slow but progressive rounding of the shoulders and loss of height. Particularly devastating seem to be hip fractures – up to one third of patients never seem to regain full mobility.
Cardiovascular risks *
It is now well accepted that women’s risk of atherosclerosis (hardening of the arteries) increases after menopause. Estrogen replacement therapy seems to reverse this trend. New evidence suggests that a similar phenomenon occurs in men as their testosterone levels diminish with age. While research is not as complete as for women, the clinical findings point to an association between low testosterone levels and an increase in cardiovascular risk factors in men.
* A cause and effect relationship has not yet been established in large clinical trials. The current clinical work does support further research into this important area of study.
What can you do about Andropause?
1- Understand your own risks for osteoporosis.
It is impossible to predict who will get osteoporosis. However, there are several factors that can put certain men at increased risk. These include:
- Age
- Low testosterone levels
- Family history of osteoporosis
- Thin and/or small frame
- Use of certain medications such as corticosteroids, anticonvulsants and anti-rejection drugs
- Excessive alcohol consumption
- Smoking
- Lack of weight-bearing exercise
If you have any of these risk factors you may want to find out more about osteoporosis prevention from your physician or from other providers of information on osteoporosis.
2- Talk to your physician about the role testosterone replacement therapy can play.
Just as with estrogen replacement therapy in women with menopause, testosterone replacement in men with Andropause has been shown to be highly effective and very beneficial. Its not for every man, of course, even men who have the symptoms on the previous quiz may have other health problems at the root of it all. Testosterone replacement therapy is a good solution for many men who are experiencing symptoms that are having an affect on their enjoyment of life.
Your doctor will check carefully to see if you are a suitable candidate, including performing blood tests and physical examinations. Importantly, if you have an established prostate tumor or have breast cancer you will not be a candidate for testosterone replacement therapy. If you are a candidate for testosterone replacement therapy the options include oral capsules, injections and skin patches. Expect your physician to monitor your progress and your overall health while on testosterone treatment. If you’re like the majority of men, you will experience very few side effects, if any.
3- Maintain a healthy lifestyle
Of course, any ongoing strategy to reduce the symptoms and risks of Andropause should incorporate lifestyle approaches such as optimal diet, regular exercise, stress-management, and the reduction in tobacco and alcohol intake.
What should I expect from testosterone replacement?
Very good responses to testosterone have been reported for men with low testosterone in various clinical studies and they include:
- Improvement in mood and sense of well-being
- Increased mental and physical energy
- Decreased anger, irritability, sadness, tiredness, nervousness
- Improved quality of sleep
- Improved libido and sexual performance
- A decline in biochemical markers of bone degradation and an increase in bone density
- An increase in lean body mass, a decline in fat mass
- An increase in muscle strength (hand grip, upper and lower extremities).
- Potentially, a decrease in the risk of heart disease
With testosterone therapy, one’s attitude improves, reinforcing self-esteem and self-confidence in success at work, and increased energy at home and in social activities. Most men will feel more vigorous, experience improvement in energy levels, mood, concentration, cognition, libido, sexual performance and overall sense of well-being. This effect is usually noted in 3 to 6 weeks. Other potential benefits include maintenance or improvement in bone density, improved body composition, muscle mass and muscle strength, as well as improvement in visual-spatial skills.
Questions and Answers
Q: Does Viagra have the same actions as testosterone?
A: It is testosterone that is the normal basis of sexual desire in both men and women. So if it is low, so is the desire for sex. Viagra is not a testosterone replacement therapy and it is prescribed to help maintain erections. It does not treat the whole man. Other symptoms such as reduced mental and physical energy, irritability and sweating may also impact your sex life. And these symptoms may also be caused by a decline in your testosterone level. So talk to your doctor about choosing the strategy that’s right for you to improve your sexual well-being.
Q: I am already taking so many medications for this and that. Should I learn to age gracefully without taking any more medicines?
A: It took many years for women to accept hormone replacement therapy. Estrogens are known to offer postmenopausal women many physical benefits, improve their psychological well-being, and therefore their overall quality of life, going full charge to the end.
Q: I am 72 years old. Am I too old to start testosterone therapy?
A: No patient is too old to start testosterone therapy if it is clearly indicated. As for any medication, testosterone should be taken under a physician’s care, with regular appropriate follow-up evaluations.
Q: Does having to take testosterone mean I’m somehow less ‘manly’?
A: Not at all. In fact, even the most “macho” men can develop this condition.
Q: Doesn’t testosterone make men aggressive and hostile?
A: Because of reports of the abuse of anabolic steroids by athletes, testosterone has suffered a negative public image. The perception is that testosterone is responsible for undesirable male traits such as aggression and hyper-sexuality. And some people have developed a fear that it will “bring out the beast in men”. These, of course, are myths. They stem from results of testosterone being used by men with normal testosterone levels who took testosterone at doses which were much higher than supplementation doses that are used in men
going through Andropause.
Q: I have been diagnosed with prostate cancer. Can I take testosterone?
A: No. In men who have an existing cancer of the prostate testosterone can promote its growth. This is why testosterone replacement is
not recommended for men with prostate cancer.
Q: I have an enlarged prostate. Can I take testosterone?
A: The prostate slowly enlarges as men age. And in some men, testosterone can cause this process to speed up. However, in most studies, no growth was found – even after long-term testosterone replacement. Consequently, some men with enlarged prostates can qualify for testosterone therapy, but others do not. Only a physician can make the decision of whether you qualify. If you do take testosterone replacement your physician will monitor the health of your prostate with regular (PSA) blood tests and physical examinations.